
A narrative review on the implementation of liquid biopsy as a diagnostic tool in thoracic tumors during the COVID-19 pandemic
Introduction
To date, severe acute respiratory syndrome (SARS-CoV-2) coronavirus has infected about 87 million people worldwide. First reported in Wuhan, China, in mid December 2019, it soon swept across China and the rest of the world (1). On January 30, 2020, the World Health Organization (WHO) declared the SARS-CoV-2 outbreak a public health emergency. However, a few months later, owing to its unstoppable spread, it was labeled as a global pandemic in a virtual media briefing on coronavirus disease 2019 (COVID-19) (2). During the first wave of the pandemic, endeavouring to thwart the spread of the disease, governments across the globe imposed state lockdowns. Such drastic measure completely upended social and economic activities. Indeed, most productive activities, including academic teaching and research, were suspended. Making matters worse was the sudden surge in SARS-CoV-2 patients needing medical assistance, ranging from primary care to intensive care. In the wake of such scenario, all international health systems were soon overwhelmed. Indeed, many hospital buildings were converted into COVID-19 facilities to withstand the substantial influx of infectious cases (3). Moreover, the massive recruitment of energy and healthcare human resources needed to cope with the pandemic determined a series of delays in diagnosis and treatments, as well as suspension of follow-up care for many patients with chronic conditions (4). Consequently, whereas medical diagnostic activities, classified as non-urgent, were significantly modified, novel workflows for the management of oncological patients were adopted by many clinics to ensure adequate clinical triage.
The field of predictive molecular pathology was also swept in this scenario. Pinto et al. reported that molecular tests decreased by 27% in the period from March 16 to April 15, 2020, compared to the same period in 2019. Stunningly, liquid biopsy testing for the detection of epidermal growth factor receptor (EGFR) exon 20 p.T790M decreased by about 67% (5). Interestingly, in a recent study, which compared our molecular testing volume during lockdown with that of the corresponding period in 2019, Malapelle et al. reported not only a reduction in liquid biopsy samples but also a change in the laboratory organization. For example, fully automated technologies, such as the Idylla platform, were introduced to offset limited staff and work hours (6). One of the most important lessons our laboratory learned from the first wave of COVID-19 is that however drastic government restrictions may be during a health emergency, no patient should ever be left behind. Now that the world is the midst of a second wave of the COVID-19 pandemic, a possible alternative to using conventional tissue or cytological samples for molecular predictive purposes could be the adoption of liquid biopsy. Indeed, being a rapid, valid, and minimally invasive approach, it is now increasingly being used in everyday clinical practice to identify predicting biomarkers in a high percentage of lung cancer patients (7). In particular, circulating tumor DNA (ctDNA) consists of small fractions of whole cell-free DNA (cfDNA) that are released into the bloodstream by tumor cells through either active or passive mechanisms. As of today, even though several promising biomarkers have been isolated from torrent blood (cfDNA, extracellular vesicle, miRNA), only ctDNA is currently approved for the administration of targeted therapies (8). However, ctDNA has yet to be approved as a predictive biomarker for treatment selection in non-small cell lung cancer (NSCLC) patients. In this review, we evaluate the role of liquid biopsy in managing lung cancer patients during the still ongoing COVID-19 healthcare emergency (Figure 1).
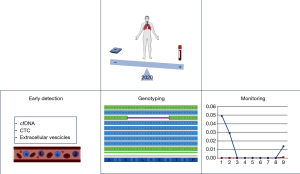
We present the following article, as a result of a deep analysis of the recent international literature published in English on PubMed in the last six months focused on the impact of SARS-CoV-2 on the management of lung cancer patients, focusing the attention on the role of liquid biopsy, in accordance with the Narrative Review Reporting Checklist (available at: https://dx.doi.org/10.21037/med-21-9).
Liquid biopsy: general considerations
Studies have shown that ctDNA has a very short half-life and circulates in the bloodstream at very low concentrations. Therefore, appropriate pre-clinical management of ctDNA in liquid biopsy is crucial to preserve its stability (9). In this regard, sample collection and storage are two fundamental pre-analytical steps. For example, when BD Vacutainer® blood collection tubes are used, it is mandatory to clarify plasma and store the supernatant at −20 °C within 2 hours from blood draw. However, when commercially available preservative tubes are used, stability can be maintained for much longer periods of time, even up to seven days from blood draw. Another important pre-analytical step is sampling time. In fact, ctDNA concentration is higher in advanced than in early stage cancer patients (10). Moreover, plasma is generally preferred to serum for clinical applications (11-13).
In spite of these few technical issues, liquid biopsy is a valid alternative to other types of conventional tissue and cytological samples in the advanced stages of cancer to select patients for targeted therapies. Indeed, NSCLC patients harboring EGFR- sensitizing mutations in liquid biopsy benefit from EGFR tyrosine kinase inhibitors (TKIs) administration. For instance, our laboratory recently showed an overall EGFR mutation detection rate of 8% from ctDNA prospectively analyzed and extracted from the plasma of advanced NSCLC patients (14,15). In all instances, all EGFR mutations were also further confirmed by an orthogonal digital polymerase chain reaction (dPCR) assay. Evidence for the utility of plasma ctDNA as a predictive biomarker in NSCLC patients has also emerged from the ASSES clinical trial. In this trial, the authors compared plasma ctDNA yield with that from tissue and cytological samples. Notably, findings from this trial confirmed the clinical usefulness of plasma-derived ctDNA samples, as shown by the good concordance rate with as many as 1,162 matched tissue/cytology samples (16).
Equally important, liquid biopsy has also been implemented in clinical trials to assess the development of drug resistance. For instance, the AURA trial demonstrated the efficiency of liquid biopsy specimens in routine clinical practice to identify EGFR exon 20 p.T790M resistance point mutation after first- or second-line EGFR TKIs (17). Similarly, Hochmair et al. showed a higher number of EGFR exon 20 p.T790M resistant point mutations in liquid biopsy samples than in corresponding tissue specimens (18). The comparable efficiency between this approach and tissue biopsy was also confirmed by another study showing that all plasma samples captured EGFR exon 20 p.T790M mutations, whereas only 55% of matching tissue samples did (19).
In addition to detecting mutations in the advanced stages of the disease, in recent years, liquid biopsy has also shown promise in detecting tumor-associated mutations in the very early stages of NSCLC. For example, Pérez-Ramírez et al. reported an overall detection rate in 80% of ctDNA from early stage cancer patients, despite low levels of ctDNA in the bloodstream (20). Similarly, Chen et al. demonstrated the utility of liquid biopsy in patients with stages IA-IIIA NSCLC, highlighting once again the feasibility of ctDNA identification in early stage NSCLC patients (21). Moreover, Sorber et al. demonstrated that the application of high sensitive multiplexed PCR and next generation sequencing platforms to liquid biopsy enables higher detection rates of cancer driver mutations in the early stages of the disease (22). These results clearly endorse the incorporation of this approach in routine clinical practice for early screening and detection of NSCLC and other types of solid tumors.
Circulating tumor cells are also emerging as a valuable tool for monitoring disease progression and treatment response to first line TKI EGFR treatments in NSCLC patients. Indeed, several investigators have turned their attention to the possibility of using liquid biopsy to assess minimal residual disease (MRD) after TKI treatment. In this setting, identification of molecular alterations in ctDNA may represent a good strategy to assist clinicians in choosing the best therapeutic strategy in a short amount of time. For example, Chaudhuri et al. analyzed 255 liquid biopsy samples from 40 NSCLC first line patients and 54 samples from healthy donors (23). Overall, ctDNA was detectable in 94% of blood samples from NSCLC patients. Likewise, Chae et al., in a review on the recent advances in sequencing technology and ctDNA analysis, concluded that the combination of sequencing technology and plasma ctDNA analysis can help clinicians monitor patients’ disease burden after surgical resection while assessing molecular targets, without having to recur to additional surgical treatments (24). In the future, liquid biopsy may also play a pivotal role in guiding the administration of targeted therapies in several other types of solid tumors (25).
In addition to blood samples, the presence of ctDNA has also been detected in various body fluids, such as pleura effusions, saliva, urine, and cerebrospinal fluids (26). For example, one study by Du et al. showed that quantitative PCR was able to detect EGFR mutations in 591 pleural effusions from NSCLC patients. Another study showed similar results in saliva (27). In particular, the authors successfully isolated genetic material from the saliva of patients diagnosed with NSCLC, pancreatic cancer, breast cancer, gastric cancer, and head and neck squamous cell carcinoma (28). Still, Pu et al. obtained a perfect EGFR mutation concordance between 17 saliva samples and corresponding resected samples from NSCLC patients (29).
Urinary ctDNA liquid biopsy also holds a great diagnostic potential in a variety of cancers. As evidenced by Jain et al., ctDNA isolated from urine can be useful not only to detect urological-neoplasms, but also to monitor populations at increased risk for other types of cancers, like nasopharyngeal carcinoma, gastric cancer, NSCLC, and hepatocellular carcinoma (30).
Undoubtedly, plasma ctDNA, together with other types of non-blood body fluids, constitutes a clinically valid tissue surrogate, especially in hard-to reach primary tumors or in metastatic tumors whose origin is uncertain, However, as of today, implementing liquid biopsy on a large scale in diagnostic routine remains a challenge. Indeed, a major hurdle is the high sensitivity and specificity technologies required for molecular analyses. Among these, real-time PCR (RT-PCR) is the most widely adopted laboratory technology in the clinical setting (31). Another equally valid technology is digital PCR (dPCR). Impressively, this assay can identify and quantify different mutations at the single-molecule level. For example, Malapelle et al. showed that dPCR is highly sensitive for EGFR mutations in NSCLC patients (32). A similar line of research, comparing the sensitivity of dPCR with that of an ultra-deep massive parallel sequencing, confirmed the efficiency of dPCR in detecting clinically relevant mutations, as evidenced by the high concordance rate (91.5%) between the two assays (33). Another valuable technology is NGS technology. Based on massive and parallel sequencing, this technology enables molecular cytopathologists to analyze different gene targets for different patients in a single run (34,35). Interestingly, several commercial approaches are currently available to analyze clinically relevant mutations in liquid biopsy specimens. For instance, Heeke et al. compared their in-house platform with an outsourced platform to analyze ctDNA from NSCLC patients. To this aim, they analyzed blood samples from 24 untreated non-squamous cell lung carcinoma patients with their in-house approach, namely the Oncomine cfTNA assay (Thermo Fisher Scientific, Waltham, MA, USA). Concomitantly, the same analysis was conducted by an external testing center with the Foundation Liquid test (Foundation Medicine, Cambridge, MA, USA) (36). The data showed an overall concordance between the two panels of 73%, suggesting that liquid biopsies can be efficiently analyzed by both in-house approaches and outsourced assays. In a study by Li et al. NSCLC, plasma samples were prospectively collected and analyzed by ultra-deep NGS approach by using a hybrid panel covering 37 lung cancer-related genes (37). The Authors showed a concordance of 98% between the NGS approach and digital droplet PCR (ddPCR) for EGFR and Kirsten Rat Sarcoma Viral Oncogene Homolog (KRAS) mutation analysis. Inspired by these results, a number of laboratories have developed custom panels able to satisfy their local diagnostic requests. For instance, Schwartzberg et al. recently validated a 17-gene liquid biopsy NGS panel, yielding a positive predictive value of 98.9% (38). Remarkably, in another experience, Malapelle et al. painstakingly described the development and testing efficiency of a custom NGS panel for cfDNA analysis extracted from serum and plasma specimens of 79 NSCLC patients, demonstrating a sensitivity of 90.5% and a specificity of 100% (39).
Liquid biopsy: pre-analytical and analytical issues
The COVID-19 pandemic has significantly modified our lives, including molecular laboratory practice (40). SARS-CoV-2 belongs to risk group 3 human pathogen because of its ability to generate a life-threatening infection for which satisfactory prophylaxis and treatment are still limited (41-43). Consequently, the need to ensure social distancing and security measures has led to a reduced laboratory staff. As a result, many molecular cytopathology laboratories have had to rapidly shift from more complex and time-consuming technologies to less complex and fully automated platforms, which generally require less hands-on time and expertise (6,41-43).
Undoubtedly, laboratory professionals, owing to the nature of their work, are at a higher risk of being exposed to viruses in normal times, let alone in times of a pandemic. Therefore, since the beginning of the current pandemic, several security measures have been adopted by laboratories worldwide to prevent the spread of the virus in the work environment. For example, guidelines recommend that samples from the airways, which may contain viable and transmissible viruses, be handled very carefully to avoid contagion (44-46). Regarding liquid biopsy samples, however, there is still little evidence on whether they may also represent a possible means of transmission (47). Under all circumstances, studies recommend the adoption of procedures equivalent to Biosafety Level (BSL) 2 to reduce the risk of spreading the infection among laboratory staff (46,48). In addition, adequate personal protective equipment (PPE) should be worn whenever fresh or unfixed samples are handled (49). Equally important, laboratory procedures prone to generate droplets (including sample preparation, aliquoting of material, centrifugation and vortexing) should be avoided as much as possible. However, should these highly risky procedures be unavoidable, class I or, preferably class II biosafety cabinets (BSCs) (48,50,51) are strongly recommended. Last but not least, all surface areas should be thoroughly and adequately disinfected with chemical substances with well-known activity against SARS-CoV-2 (48).
Abiding by these security measures is paramount not only to prevent laboratory professionals from contracting the infection but, equally important, to ensure that patients with diagnosed or suspected cancers continue to receive all the necessary care and services without the risk of being exposed to COVID-19. Indeed, as strongly recommended by the European Society for Medical Oncology (ESMO), lung cancer molecular analysis and treatments should be continued without any delays (52), mainly because such delays could not only worsen patients’ conditions but also create unmanageable backlogs in treatments and diagnoses.
On the other hand, the “draconian” measures adopted by state governments since the beginning of the pandemic to tackle the relentless spread of COVID-19, have reduced hospital admissions of lung cancer patients (53). In addition, the so-called “distraction effect”, due to the recruitment of healthcare figures to cope with the spread of COVID-19, has reduced the number of requests for molecular testing (54). Consequently, the limited access to diagnostic procedures has determined scarce availability of tissue samples from lung cancer patients, primarily because of the risks associated with airway tissue samples (55-57).
In this healthcare emergency, it is no wonder that liquid biopsy has recently gained increasing attention compared to more conventional tissue and cytology techniques. For example, it may be a valid option to reduce the potential risks of contagion among lung cancer patients by limiting the number of hospital stays. It could also help cytopathologists overcome some of the shortcomings associated with tissue biopsies, including the unavailability of tissue specimens for molecular purposes. Further, it could minimize the risk of handling potentially infectious airway tissue samples, thereby avoiding a potential spread of the virus among staff (58). Besides these advantages, recent research has also fully validated the efficiency of this approach in detecting cancer driver mutations both in early and in late stage lung cancer patients. This is a paramount advantage when one considers the widespread postponement of cancer screening programs. In this regard, it has been widely demonstrated that the integration of ctDNA and tumor tissue analysis into routine clinical practice may increase the detection of clinical relevant biomarkers useful for targeted treatment administration (59). In addition, the adoption of the “blood-first” approach may significantly shorten time to treatment, counterbalancing the possible delays associated with COVID-19 containment measures (60). Oddly, although Malapelle et al. reported no significant differences in the number of tested samples for molecular predictive purposes between 2019 and 2020, they did observe a significant reduction in liquid biopsies analysis (6). Plausibly, the lower volume of processed liquid biopsy samples was ascribable, on one hand, to patients’ reluctance to visit hospitals for fear of contracting the virus, and, on the other hand, to the drop in scheduled hospital appointments to ensure social distancing. Intriguingly, to circumvent this limitation, Rolfo et al. recently proposed a shift in the current diagnostic workflow of liquid biopsy samples, emphasizing the need of implementing home phlebotomy services and/or mobile units for blood draws and transport, followed by a central NGS analysis of ctDNA (58). Finally, this new approach could also be applied to monitor the efficacy of systemic treatments, including targeted drugs, and to modify the way clinical trials are carried out, especially during the current pandemic (58).
Liquid biopsy: clinical considerations
COVID-19 patients with comorbidities, including cardiopathies, diabetes, and cancer, may be at higher risk of developing life-threatening complications like cute respiratory distress syndrome (ARDS) and multiple organ failure (61). Cancer patients, especially those undergoing treatment, seem to fare worse than others (62). The reason is that tumors and the adverse effects of oncological treatments can compromise patients’ immune systems, rendering them more severely susceptible to COVID-19 infection and complications (63). Indeed according to a nationwide analysis of Chinese cancer patients during the COVID-19 outbreak, cancer patients were more vulnerable to severe events than cancer-free patients, as evidenced by the higher number of oncological patients in intensive care units needing mechanical ventilation. In addition, more severe events were seen in patients who had been on oncological active treatment for at least a month before the infection (62). Consistently, Zhang et al also showed that cancer patients affected by COVID-19, who had received antitumor therapy within 14 days of COVID-19 diagnosis, had poorer outcomes than the otherwise healthy patients (64).
Management and diagnosis of lung cancer patients during the current pandemic have been much more challenging than ever before in both intensive and a primary care settings. The reason is that COVID-19 common presenting symptoms (e.g., dyspnea, fatigue, fever, cough, and anosmia) are also very frequently found in lung cancer patients (65). Moreover, symptom overlap between thoracic malignancies and COVID-19 can complicate cancer early diagnosis in patients presenting acute symptoms (65). As mentioned earlier, in this challenging subset of SARS-CoV-2 infection, the various comorbidities associated with lung cancer can significantly affect COVID-19-related mortality risk. Among these events are cardiovascular disease, diabetes, smoking habits, and chronic obstructive pulmonary disease (COPD) (66). Thus, lung cancer patients are particularly vulnerable to suffering from respiratory failure due to SARS-CoV-2-related pneumonia (67,68). Specifically, in a large multicenter observational study (the TERAVOLT trial), a higher mortality risk was statistically and clinically associated with age, smoking status, chemotherapy treatment, and the concomitant presence of comorbidities (68).
Hence, although this unprecedented global scenario has significantly affected the routine clinical management of lung cancer patients, it behooves health care professionals to continue providing personalized cancer treatments along with the best therapeutic strategies while minimizing as much as possible the risk of infection among lung cancer patients. Accordingly, different oncology societies have released several recommendations and guidelines. For instance, some guidelines recommend delaying cancer treatments on the basis of patients’ clinical status, prognosis, and tumor characteristics, and adopting telemedicine consultations instead of in-person visits (69). In view of prioritizing oncological treatments during a global pandemic, guidelines recommend at-home oral therapies instead of standard chemotherapy infusion to prevent patients from getting infected while being treated (70,71). Additionally, it is recommended that all elective surgeries be rescheduled to prioritize essential cancer surgeries (72).
The COVID-19 pandemic has had dramatic consequences on molecular testing for thoracic malignancies. One need only consider the decreased number of collected samples seen since the beginning of the pandemic. Indeed, access to diagnostic procedures, crucial for cancer diagnosis, has been limited in an effort to prevent the spread of COVID-19 infection in healthcare settings. In this context, molecular predictive pathology practice has seen a notable reduction especially in the NSCLC setting, where tumor genotyping is essential and mandatory for selective treatment (6,73).
The metastatic NSCLC setting epitomizes the value of implementing liquid biopsy in routine clinical practice, even more so during a health crisis, given the greater burden and the higher detection rate of ctDNA typically found in the advanced stages of the disease (12). Liquid biopsy, specifically cfDNA analysis, is a rapidly expanding and minimally invasive analysis of translational cancer research. Impressively, being a highly versatile tool in the management of lung cancer, liquid biopsy can assist clinicians in selecting targeted treatments, monitoring treatment response, and detecting drug resistance mechanisms, without posing the risks of contagion. For instance, studies have shown that in combination with NGS technologies, it can successfully identify therapeutically-targetable alterations, thereby improving molecularly-guided oncological treatments (74).
Therefore, in this unprecedented health emergency, the integration of liquid biopsy in routine clinical practice is crucially important to minimize the danger of SARS-CoV-2 infection for oncological patients and to reduce surgical procedures in patients with insufficient or unavailable cancer tissue for molecular analysis. Moreover, the implementation of plasma NGS jointly with tumor tissue genotyping has been demonstrated to increase mutation detection up to 26% compared with standard-of-care approaches (75). Moreover, the identification of circulating biomarkers has also be shown to guide treatment planning for a large number of patients potentially eligible for targeted oral agents. Concomitantly, it has proven highly efficient in monitoring patients undergoing active cancer treatments (76).
Interestingly, liquid biopsy can also be exploitable in the clinical trial setting. Indeed, being less invasive, easier to handle, and faster to process than conventional tissue and cytological specimens, it can help clinicians accelerate screening and enrollment of larger numbers of patients who could benefit from entering clinical trials. By the same token, integrating liquid biopsy in the current workflow may enable patients to start oncological treatment much sooner (60).
The feasibility of using liquid biopsy in clinical trials is particularly relevant in today’s health crisis. Several studies have indeed well-established that the routine conduction of clinical trials has been considerably altered since the introduction of the drastic containment measures. However, because this unprecedented clinical scenario is rapidly evolving, there is an urgent need to find dynamic alternatives to the ways clinical studies and sample collection are carried out. All things considered, a variation in regular diagnostic management for advanced lung cancer patients is highly recommended.
More specifically, before the pandemic, liquid biopsy rapidly emerged as a potential diagnostic tool able to detect and assess the earlier stages of the disease as well as post-treatment molecular residual disease (77). With the advent of the pandemic, however, cancer prevention has been overshadowed by the various response measures against the spread of COVID-19. Indeed, the pandemic has led to the suspension of cancer screening services, delayed diagnosis, and, ultimately, reduced overall cancer survival (78). In this context, liquid biopsy could be used to circumvent the delays compromising traditional screening programs while reducing the risk of viral contagion during standard procedures. Notwithstanding, future research on the possible applications of liquid biopsy in the early-stage setting is keenly warranted.
Conclusions
COVID-19 pandemic has significantly modified our lives and overall medical practice (79-81). In these unprecedented times, liquid biopsy may represent a valid and less time-consuming diagnostic approach than conventional tissue and cytological specimens. This primarily because it can help reduce the danger of viral spread by avoiding invasive surgical procedures in those NSCLC patients with insufficient or unavailable cancer tissue for molecular analysis. Furthermore, this new approach may be significantly useful not only to help oncologists choose targeted treatments according to the molecular profile of each patient’s tumor, but also to restart the many suspended clinical trials. Thus, considering today’s turbulent times and despite the practical advantages that liquid biopsy may offer, further studies are needed for the application of this non invasive approach in everyday clinical practice, as well as in clinical trials, to streamline tumor genotyping and targeted therapies.
Acknowledgments
VG and MLM contributed to the current work under the Doctoral Program in Experimental Oncology and Surgery, University of Palermo. We thank Dr. Paola Merolla for editing the manuscript.
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Giuseppe Banna and Alfredo Addeo) for the series “Changes in management of mediastinal tumours following the surge of COVID-19 pandemic” published in Mediastinum. The article has undergone external peer review.
Reporting Checklist: The authors have completed the Narrative Review Reporting Checklist. Available at: https://dx.doi.org/10.21037/med-21-9
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at: https://dx.doi.org/10.21037/med-21-9). The series “Changes in management of mediastinal tumours following the surge of COVID-19 pandemic” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Andersen KG, Rambaut A, Lipkin WI, et al. The proximal origin of SARS-CoV-2. Nat Med 2020;26:450-2. [Crossref] [PubMed]
- Cucinotta D, Vanelli M. WHO Declares COVID-19 a Pandemic. Acta Biomed 2020;91:157-60. [PubMed]
- Williams S, Tsiligianni I. COVID-19 poses novel challenges for global primary care. NPJ Prim Care Respir Med 2020;30:30. [Crossref] [PubMed]
- Hamilton W. Cancer diagnostic delay in the COVID-19 era: what happens next? Lancet Oncol 2020;21:1000-2. [Crossref] [PubMed]
- Pinto Daniel. How the COVID-19 Pandemic Impacted Oncological Molecular Diagnosis: A Picture from a National Reference Center for Molecular Pathology. Biomed Res Int 2020;2020:8397053 [PubMed]
- Malapelle U, De Luca C, Iaccarino A, et al. Predictive molecular pathology in the time of COVID-19. J Clin Pathol 2021;74:234-7. [Crossref] [PubMed]
- Pisapia P, Malapelle U, Troncone G. Liquid Biopsy and Lung Cancer. Acta Cytol 2019;63:489-96. [Crossref] [PubMed]
- Jia S, Zhang R, Li Z, et al. Clinical and biological significance of circulating tumor cells, circulating tumor DNA, and exosomes as biomarkers in colorectal cancer. Oncotarget 2017;8:55632-45. [Crossref] [PubMed]
- Kustanovich A, Schwartz R, Peretz T, et al. Life and death of circulating cell-free DNA. Cancer Biol Ther 2019;20:1057-67. [Crossref] [PubMed]
- Koncina E, Haan S, Rauh S, et al. Prognostic and Predictive Molecular Biomarkers for Colorectal Cancer: Updates and Challenges. Cancers (Basel) 2020;12:319. [Crossref] [PubMed]
- Poulet G, Massias J, Taly V. Liquid Biopsy: General Concepts. Acta Cytol 2019;63:449-55. [Crossref] [PubMed]
- Rolfo C, Mack PC, Scagliotti GV, et al. Liquid Biopsy for Advanced Non-Small Cell Lung Cancer (NSCLC): A Statement Paper from the IASLC. J Thorac Oncol 2018;13:1248-68. [Crossref] [PubMed]
- Rolfo C, Cardona AF, Cristofanilli M, et al. Challenges and opportunities of cfDNA analysis implementation in clinical practice: Perspective of the International Society of Liquid Biopsy (ISLB). Crit Rev Oncol Hematol 2020;151:102978 [Crossref] [PubMed]
- Pisapia P, Pepe F, Smeraglio R, et al. Cell free DNA analysis by SiRe® next generation sequencing panel in non small cell lung cancer patients: focus on basal setting. J Thorac Dis 2017;9:S1383-90. [Crossref] [PubMed]
- Nacchio M, Sgariglia R, Gristina V, et al. KRAS mutations testing in non-small cell lung cancer: the role of Liquid biopsy in the basal setting. J Thorac Dis 2020;12:3836-43. [Crossref] [PubMed]
- Arriola E, Paredes-Lario A, García-Gomez R, et al. Comparison of plasma ctDNA and tissue/cytology-based techniques for the detection of EGFR mutation status in advanced NSCLC: Spanish data subset from ASSESS. Clin Transl Oncol 2018;20:1261-7. [Crossref] [PubMed]
- Yang JC, Ahn MJ, Kim DW, et al. Osimertinib in Pretreated T790M-Positive Advanced Non-Small-Cell Lung Cancer: AURA Study Phase II Extension Component. J Clin Oncol 2017;35:1288-96. [Crossref] [PubMed]
- Hochmair MJ, Buder A, Schwab S, et al. Liquid-Biopsy-Based Identification of EGFR T790M Mutation-Mediated Resistance to Afatinib Treatment in Patients with Advanced EGFR Mutation-Positive NSCLC, and Subsequent Response to Osimertinib. Target Oncol 2019;14:75-83. [Crossref] [PubMed]
- Li C, Jia R, Liu H, et al. EGFR T790M detection and osimertinib treatment response evaluation by liquid biopsy in lung adenocarcinoma patients with acquired resistance to first generation EGFR tyrosine kinase inhibitors. Diagn Pathol 2018;13:49. [Crossref] [PubMed]
- Pérez-Ramírez C, Cañadas-Garre M, Robles AI, et al. Liquid biopsy in early stage lung cancer. Transl Lung Cancer Res 2016;5:517-24. [Crossref] [PubMed]
- Chen K, Kang G, Zhao H, et al. Liquid biopsy in newly diagnosed patients with locoregional (I-IIIA) non-small cell lung cancer. Expert Rev Mol Diagn 2019;19:419-27. [Crossref] [PubMed]
- Sorber L, Zwaenepoel K, Deschoolmeester V, et al. Circulating cell-free nucleic acids and platelets as a liquid biopsy in the provision of personalized therapy for lung cancer patients. Lung Cancer 2017;107:100-7. [Crossref] [PubMed]
- Chaudhuri AA, Chabon JJ, Lovejoy AF, et al. Early Detection of Molecular Residual Disease in Localized Lung Cancer by Circulating Tumor DNA Profiling. Cancer Discov 2017;7:1394-403. [Crossref] [PubMed]
- Chae YK, Oh MS. Detection of Minimal Residual Disease Using ctDNA in Lung Cancer: Current Evidence and Future Directions. J Thorac Oncol 2019;14:16-24. [Crossref] [PubMed]
- Saarenheimo J, Eigeliene N, Andersen H, et al. The Value of Liquid Biopsies for Guiding Therapy Decisions in Non-small Cell Lung Cancer. Front Oncol 2019;9:129. [Crossref] [PubMed]
- Siravegna G, Marsoni S, Siena S, et al. Integrating liquid biopsies into the management of cancer. Nat Rev Clin Oncol 2017;14:531-48. [Crossref] [PubMed]
- Du Y, Guo X, Wang R, et al. The Correlation between EGFR Mutation Status and DNA Content of Lung Adenocarcinoma Cells in Pleural Effusion. J Cancer 2020;11:2265-72. [Crossref] [PubMed]
- Kaczor-Urbanowicz KE, Wei F, Rao SL, et al. Clinical validity of saliva and novel technology for cancer detection. Biochim Biophys Acta Rev Cancer 2019;1872:49-59. [Crossref] [PubMed]
- Pu D, Liang H, Wei F, et al. Evaluation of a novel saliva-based epidermal growth factor receptor mutation detection for lung cancer: A pilot study. Thorac Cancer 2016;7:428-36. [Crossref] [PubMed]
- Jain S, Lin SY, Song W, et al. Urine-Based Liquid Biopsy for Nonurological Cancers. Genet Test Mol Biomarkers 2019;23:277-83. [Crossref] [PubMed]
- Mayo-de-Las-Casas C, Garzón Ibáñez M, Jordana-Ariza N, et al. An update on liquid biopsy analysis for diagnostic and monitoring applications in non-small cell lung cancer. Expert Rev Mol Diagn 2018;18:35-45. [Crossref] [PubMed]
- Malapelle U, de Luca C, Vigliar E, et al. EGFR mutation detection on routine cytological smears of non-small cell lung cancer by digital PCR: a validation study. J Clin Pathol 2016;69:454-7. [Crossref] [PubMed]
- Tran LS, Pham HT, Tran VU, et al. Ultra-deep massively parallel sequencing with unique molecular identifier tagging achieves comparable performance to droplet digital PCR for detection and quantification of circulating tumor DNA from lung cancer patients. PLoS One 2019;14:e0226193 [Crossref] [PubMed]
- Rothberg JM, Hinz W, Rearick TM, et al. An integrated semiconductor device enabling non-optical genome sequencing. Nature 2011;475:348-52. [Crossref] [PubMed]
- Bentley DR, Balasubramanian S, Swerdlow HP, et al. Accurate whole human genome sequencing using reversible terminator chemistry. Nature 2008;456:53-9. [Crossref] [PubMed]
- Heeke S, Hofman V, Ilié M, et al. Prospective evaluation of NGS-based liquid biopsy in untreated late stage non-squamous lung carcinoma in a single institution. J Transl Med 2020;18:87. [Crossref] [PubMed]
- Li BT, Janku F, Jung B, et al. Ultra-deep next-generation sequencing of plasma cell-free DNA in patients with advanced lung cancers: results from the Actionable Genome Consortium. Ann Oncol 2019;30:597-603. [Crossref] [PubMed]
- Schwartzberg LS, Horinouchi H, Chan D, et al. Liquid biopsy mutation panel for non-small cell lung cancer: analytical validation and clinical concordance. NPJ Precis Oncol 2020;4:15. [Crossref] [PubMed]
- Malapelle U, Mayo de-Las-Casas C, Rocco D, et al. Development of a gene panel for next-generation sequencing of clinically relevant mutations in cell-free DNA from cancer patients. Br J Cancer 2017;116:802-10. [Crossref] [PubMed]
- Bardelli A. Coronavirus lockdown: What I learnt when I shut my cancer lab in 48 hours. Nature 2020; Epub ahead of print. [Crossref] [PubMed]
- Barbareschi M, Ascoli V, Bonoldi E, et al. Biosafety in surgical pathology in the era of SARS-Cov2 pandemia. A statement of the Italian Society of Surgical Pathology and Cytology. Pathologica 2020;112:59-63. [PubMed]
- Iwen PC, Stiles KL, Pentella MA. Safety Considerations in the Laboratory Testing of Specimens Suspected or Known to Contain the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2). Am J Clin Pathol 2020;153:567-70. [Crossref] [PubMed]
- Health and safety executive advisory committee on dangerous pathogens. The Approved list of biological agents. Secondary the Approved list of biological agents. [accessed on 2021 Jan 9]. Available online: www.hse.gov.uk/pubns/misc208.pdf
- Chen J, Lu H, Melino G, et al. COVID-19 infection: the China and Italy perspectives. Cell Death Dis 2020;11:438. [Crossref] [PubMed]
- Chen CC, Chi CY. Biosafety in the preparation and processing of cytology specimens with potential coronavirus (COVID-19) infection: Perspectives from Taiwan. Cancer Cytopathol 2020;128:309-16. [Crossref] [PubMed]
- World Health Organization (WHO). Laboratory biosafety guidance related to the novel coronavirus (2019-nCoV). Interim guidance. [accessed on 2021 Jan 9]. Available online: https://www.who.int/docs/default-source/coronaviruse/laboratory-biosafety-novel-coronavirus-version-1-1.pdf?sfvrsn=912a9847_2
- Wang W, Xu Y, Gao R, et al. Detection of SARS-CoV-2 in Different Types of Clinical Specimens. JAMA 2020;323:1843-4. [Crossref] [PubMed]
- Interim Laboratory Biosafety Guidelines for Handling and Processing Specimens Associated with Coronavirus Disease 2019 (COVID-19). Accessed on 09/01/2021. Available online: https://www.cdc.gov/coronavirus/2019-ncov/lab/lab-biosafety-guidelines.html
- World Health Organization (WHO). Personal protective equipment for COVID-19. No Title. [accessed on 2021 Jan 9]. Available online: https://www.who.int/teams/health-product-and-policy-standards/access-to-assistive-technology-medical-devices/priority-medical-devices-for-covid/ppe-covid
- Iaccarino A, Pisapia P, Vigliar E, et al. Juggling the COVID-19 pandemic: A cytopathology point of view. Cytopathology 2021;32:299-303. [Crossref] [PubMed]
- Pisapia P, Malapelle U, Salatiello M, et al. A narrative review of lung cancer cytology in the times of coronavirus: what physicians should know. Transl Lung Cancer Res 2020;9:2074-81. [Crossref] [PubMed]
- Passaro A, Addeo A, Von Garnier C, et al. ESMO Management and treatment adapted recommendations in the COVID-19 era: Lung cancer. ESMO Open 2020;5:e000820 [Crossref] [PubMed]
- Lavazza A, Farina M. The Role of Experts in the Covid-19 Pandemic and the Limits of Their Epistemic Authority in Democracy. Front Public Health 2020;8:356. [Crossref] [PubMed]
- Cortiula F, Pettke A, Bartoletti M, et al. Managing COVID-19 in the oncology clinic and avoiding the distraction effect. Ann Oncol 2020;31:553-5. [Crossref] [PubMed]
- Vigliar E, Iaccarino A, Bruzzese D, et al. Cytology in the time of coronavirus disease (COVID-19): an Italian perspective. J Clin Pathol 2021;74:261-3. [Crossref] [PubMed]
- Vigliar E, Cepurnaite R, Alcaraz-Mateos E, et al. Global impact of the COVID-19 pandemic on cytopathology practice: Results from an international survey of laboratories in 23 countries. Cancer Cytopathol 2020;128:885-94. [Crossref] [PubMed]
- Dinmohamed AG, Visser O, Verhoeven RHA, et al. Fewer cancer diagnoses during the COVID-19 epidemic in the Netherlands. Lancet Oncol 2020;21:750-1. [Crossref] [PubMed]
- Rolfo C, Russo A, de Miguel-Pérez D. Speeding tumor genotyping during the SARS-CoV-2 outbreak through liquid biopsy. Cancer 2020;126:4089-91. [Crossref] [PubMed]
- Siravegna G, Mussolin B, Venesio T, et al. How liquid biopsies can change clinical practice in oncology. Ann Oncol 2019;30:1580-90. [Crossref] [PubMed]
- Leighl NB, Page RD, Raymond VM, et al. Clinical Utility of Comprehensive Cell-free DNA Analysis to Identify Genomic Biomarkers in Patients with Newly Diagnosed Metastatic Non-small Cell Lung Cancer. Clin Cancer Res 2019;25:4691-700. [Crossref] [PubMed]
- Torres Acosta MA, Singer BD. Pathogenesis of COVID-19-induced ARDS: implications for an ageing population. Eur Respir J 2020;56:2002049 [Crossref] [PubMed]
- Liang W, Guan W, Chen R, et al. Cancer patients in SARS-CoV-2 infection: a nationwide analysis in China. Lancet Oncol 2020;21:335-7. [Crossref] [PubMed]
- Miyashita H, Mikami T, Chopra N, et al. Do patients with cancer have a poorer prognosis of COVID-19? An experience in New York City. Ann Oncol 2020;31:1088-9. [Crossref] [PubMed]
- Zhang L, Zhu F, Xie L, et al. Clinical characteristics of COVID-19-infected cancer patients: a retrospective case study in three hospitals within Wuhan, China. Ann Oncol 2020;31:894-901. [Crossref] [PubMed]
- Bakhribah H, Zeitouni M, Daghistani RA, et al. Implications of COVID-19 pandemic on lung cancer management: A multidisciplinary perspective. Crit Rev Oncol Hematol 2020;156:103120 [Crossref] [PubMed]
- Rogado J, Pangua C, Serrano-Montero G, et al. Covid-19 and lung cancer: A greater fatality rate? Lung Cancer 2020;146:19-22. [Crossref] [PubMed]
- Dai M, Liu D, Liu M, et al. Patients with Cancer Appear More Vulnerable to SARS-CoV-2: A Multicenter Study during the COVID-19 Outbreak. Cancer Discov 2020;10:783-91. [PubMed]
- Garassino MC, Whisenant JG, Huang LC, et al. COVID-19 in patients with thoracic malignancies (TERAVOLT): first results of an international, registry-based, cohort study. Lancet Oncol 2020;21:914-22. [Crossref] [PubMed]
- Tartarone A, Lerose R. COVID-19 and cancer care: what do international guidelines say? Med Oncol 2020;37:80. [Crossref] [PubMed]
- Cinar P, Kubal T, Freifeld A, et al. Safety at the Time of the COVID-19 Pandemic: How to Keep our Oncology Patients and Healthcare Workers Safe. J Natl Compr Canc Netw 2020; Epub ahead of print. [Crossref] [PubMed]
- Hanna TP, Evans GA, Booth CM. Cancer, COVID-19 and the precautionary principle: prioritizing treatment during a global pandemic. Nat Rev Clin Oncol 2020;17:268-70. [Crossref] [PubMed]
- COVID19 Subcommittee of the O.R. Executive Committee at Memorial Sloan Kettering. Cancer Surgery and COVID19. Ann Surg Oncol 2020;27:1713-6. [Crossref] [PubMed]
- Lindeman NI, Cagle PT, Aisner DL, et al. Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment With Targeted Tyrosine Kinase Inhibitors: Guideline From the College of American Pathologists, the International Association for the Study of Lung Cancer, and the Association for Molecular Pathology. Arch Pathol Lab Med 2018;142:321-46. [Crossref] [PubMed]
- Aggarwal C, Thompson JC, Black TA, et al. Clinical Implications of Plasma-Based Genotyping With the Delivery of Personalized Therapy in Metastatic Non-Small Cell Lung Cancer. JAMA Oncol 2019;5:173-80. [Crossref] [PubMed]
- Pritchett MA, Camidge DR, Patel M, et al. Prospective Clinical Validation of the InVisionFirst-Lung Circulating Tumor DNA Assay for Molecular Profiling of Patients With Advanced Nonsquamous Non-Small-Cell Lung Cancer. JCO Precis Oncol 2019;3:PO.18.00299.
- Palmirotta R, Lovero D, Cafforio P, et al. Liquid biopsy of cancer: a multimodal diagnostic tool in clinical oncology. Ther Adv Med Oncol 2018;10:1758835918794630 [Crossref] [PubMed]
- Guibert N, Pradines A, Favre G, et al. Current and future applications of liquid biopsy in nonsmall cell lung cancer from early to advanced stages. Eur Respir Rev 2020;29:190052 [Crossref] [PubMed]
- Maringe C, Spicer J, Morris M, et al. The impact of the COVID-19 pandemic on cancer deaths due to delays in diagnosis in England, UK: a national, population-based, modelling study. Lancet Oncol 2020;21:1023-34. [Crossref] [PubMed]
- Paules CI, Marston HD, Fauci AS. Coronavirus Infections-More Than Just the Common Cold. JAMA 2020;323:707-8. [Crossref] [PubMed]
- Fauci AS, Lane HC, Redfield RR. Covid-19 - Navigating the Uncharted. N Engl J Med 2020;382:1268-9. [Crossref] [PubMed]
- Morens DM, Fauci AS. Emerging Pandemic Diseases: How We Got to COVID-19. Cell 2020;182:1077-92. [Crossref] [PubMed]
Cite this article as: Pisapia P, Pepe F, Gristina V, La Mantia M, Francomano V, Russo G, Iaccarino A, Galvano A. A narrative review on the implementation of liquid biopsy as a diagnostic tool in thoracic tumors during the COVID-19 pandemic. Mediastinum 2021;5:27.


