VATS thymectomy—bilateral approach for extended resection
Evolution of bilateral VATS extended thymectomy
In the middle 1990s, VATS thymectomy procedures were attempted by several different surgeons for myasthenia gravis cases. Yim et al. started performing VATS extended thymectomy procedures in Hong Kong in 1993 and reported their experience with 8 cases in 1995 (1). In Japan, Ando et al. also reported 2 cases of bilateral VATS extended thymectomy with a cervical incision in 1996 (2). That latter study emphasized the merits of a VATS extended thymectomy in terms of less invasiveness, including reduced pain, smaller incision, and unnecessary postoperative mechanical ventilation, and also noted that a bilateral approach has an advantage of confirming the bilateral phrenic nerves. On the other hand, a disadvantage of longer operation time due to difficulty in resection of pericardial fat tissue was emphasized in the early period.
Soon after introduction of the VATS extended thymectomy procedure, an approach through the anterior cervical incision was added, because the peri-thymic tissues are thought to reside mostly around the upper poles of the thymus. In 1998, Mantegazza et al. reported that the 2-year outcomes of bilateral VATS extended thymectomy cases with a cervical approach were comparable with those of a trans-sternal extended thymectomy (3). Later, in 2003, the same group again reported a 6-year complete remission rate of non-thymomatous MG patients of 50.6% after VATS extended thymectomy and 48.7% after trans-sternal extended thymectomy, which were not significantly different (4).
An important breakthrough was achieved by introducing elevation of the sternum with several different methods reported in the 2000’s, mainly in Japan (5-9). Our group at the Department of General Thoracic Surgery of Osaka University Hospital has presented progress with bilateral VATS extended thymectomy techniques in serial publications. Our own method for lifting the anterior chest wall is shown in Figure 1 (9,10), in which the original costal hooks are placed on the bilateral third ribs to maximize the operative field. Shiono et al. reported long-term outcomes of bilateral VATS extended thymectomy procedures with anterior chest wall lifting and cervical incision, including a 4-year remission rate of 44.4%, which was comparable to that reported for a trans-sternal extended thymectomy (11).
Development of bilateral VATS extended thymectomy without cervical incision
Shigemura et al. sought to determine the amounts of additional thymic or peri-thymic tissues resected through a cervical incision during bilateral thoracoscopic thymectomy procedures (12). They found that 0.8 g of thymic or peri-thymic tissue was able to be further resected by changing the head position with the neck flexed to drop the jaw onto the anterior chest. Then, cervical incision is further added, which enabled us to resect an additional 0.5 g of the tissue. Histopathologic studies have also revealed the presence of germinal centers as well as Hassall’s corpuscles in residual tissues in more than 70% of examined cases, which suggested that a VATS extended thymectomy without a cervical incision, might be an immunologically incomplete treatment for myasthenia gravis.
Later in 2011, we recognized that division of the right internal thoracic vein makes an approach to the anterior neck region from the right thorax easier, thus the transcervical approach was abandoned. Nakagiri et al. (13) reported that outcomes of bilateral VATS extended thymectomy procedures with anterior chest lifting without a transcervical approach in a flexed neck position were comparable to those noted in the previous report.
CO2 insufflation into the thoracic cavity has been introduced to improve the anterior mediastinal view. With this technique, the left brachiocephalic vein is compressed by positive pressure inside the thoracic cavity, leading to further visualization of the anterior cervical region. Chan et al. reported results of bilateral VATS thymectomy using CO2 insufflation in 2005 and noted avoidance of a cervical incision (14). Furthermore, this method has an advantage of reducing bleeding from small vessels.
Current bilateral VATS extended thymectomy method used at Osaka University Hospital
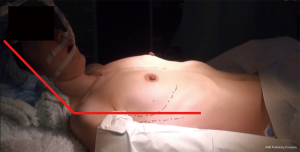
Based on the advancements noted above, the Osaka University General Thoracic Surgery group has established our current method for bilateral VATS extended thymectomy without a cervical incision (10), including patient position (Figure 2).
The techniques utilized are shown in Figures 3,4. Briefly, the procedure starts in the right thoracic cavity with creation of 3 ports, then CO2 insufflation is used to visualize the anterior mediastinum. Most of the procedures for dissecting the thymus as well as dividing the thymic veins are done from the right side, though we think that the left phrenic nerve should be confirmed from the left side. Dissection of the left lobe of the thymus is done in part from the left, though the left upper pole of the thymus is visualized more clearly and divided from the right side. Another advantage of a bilateral approach is that a better operative field can be obtained by mobilization of the thymus from the contralateral side. Lavage of the bilateral thoracic cavities is done with a physiological saline solution and hemostasis confirmed. Drainage tubes are inserted into the bilateral thoracic cavities, then the incisions are closed.


Future perspectives for bilateral VATS extended thymectomy
An advantage of a bilateral VATS extended thymectomy is ability to confirm the bilateral phrenic nerves and it seems to be the most conventional method available, though the procedure is thought to be more invasive than a unilateral approach in terms of longer procedure time and bilateral thoracic incision.
Caronia et al. reported a uniportal bilateral approach (17), in which advancement to the reduced port might be a solution to reduce the invasiveness of a bilateral VATS extended thymectomy.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors Nuria Novoa and Wentao Fang for the series “Minimally Invasive Thymectomy” published in Mediastinum. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/med.2018.04.03). The series “Minimally Invasive Thymectomy” was commissioned by the editorial office without any funding or sponsorship. MO serves as an unpaid editorial board member of Mediastinum from May 2017 - Apr 2019. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Yim AP, Kay RL, Ho JK. Video-assisted thoracoscopic thymectomy for myasthenia gravis. Chest 1995;108:1440-3. [Crossref] [PubMed]
- Andou A, Azuma T, Tsukazaki T, et al. Thoracoscopic extended thymectomy with collar incision of the neck in two patients with myasthenia gravis. J Jpn Assoc Chest Surg 1996;10:107-11. [Crossref]
- Mantegazza R, Confalonieri P, Antozzi C, et al. Video-assisted thoracoscopic extended thymectomy (VATET) in myasthenia gravis: two-year follow-up in 101 patients and comparison with the transsternal approach. Ann N Y Acad Sci 1998;841:749-52. [Crossref] [PubMed]
- Mantegazza R, Baggi F, Bernasconi P, et al. Video-assisted thoracoscopic extended thymectomy and extended transsternal thymectomy (T-3b) in non-thymomatous myasthenia gravis patients: remission after 6 years of follow-up. J Neurol Sci 2003;212:31-6. [Crossref] [PubMed]
- Kido T, Hazama K, Inoue Y, et al. Resection of anterior mediastinal masses through an infrasternal approach. Ann Thorac Surg 1999;67:263-5. [Crossref] [PubMed]
- Uchiyama A, Shimizu S, Murai H, et al. Infrasternal mediastinoscopic thymectomy in myasthenia gravis: surgical results in 23 patients. Ann Thorac Surg 2001;72:1902-5. [Crossref] [PubMed]
- Takeo S, Sakada T, Yano T. Video-assisted extended thymectomy in patients with thymoma by lifting the sternum. Ann Thorac Surg 2001;71:1721-3. [Crossref] [PubMed]
- Zieliński M, Kuzdzał J, Szlubowski A, et al. Transcervical-subxiphoid-videothoracoscopic "maximal" thymectomy—operative technique and early results. Ann Thorac Surg 2004;78:404-9; discussion 409-10. [Crossref] [PubMed]
- Ohta M, Hirabayasi H, Okumura M, et al. Thoracoscopic thymectomy using anterior chest wall lifting method. Ann Thorac Surg 2003;76:1310-1. [Crossref] [PubMed]
- Okumura M, Shintani Y, Ohta M, et al. Minimally invasive surgical procedures for thymic disease in Asia. J Vis Surg 2017;3:96. [Crossref] [PubMed]
- Shiono H, Kadota Y, Hayashi A, et al. Comparison of outcomes after extended thymectomy for myasthenia gravis: bilateral thoracoscopic approach versus sternotomy. Surg Laparosc Endosc Percutan Tech 2009;19:424-7. [Crossref] [PubMed]
- Shigemura N, Shiono H, Inoue M, et al. Inclusion of the transcervical approach in video-assisted thoracoscopic extended thymectomy (VATET) for myasthenia gravis: a prospective trial. Surg Endosc 2006;20:1614-8. [Crossref] [PubMed]
- Nakagiri T, Inoue M, Shintani Y, et al. Improved procedures and comparative results for video-assisted thoracoscopic extended thymectomy for myasthenia gravis. Surg Endosc 2015;29:2859-65. [Crossref] [PubMed]
- Chang PC, Chou SH, Kao EL, et al. Bilateral video-assisted thoracoscopic thymectomy vs. extended transsternal thymectomy in myasthenia gravis: a prospective study. Eur Surg Res 2005;37:199-203. [Crossref] [PubMed]
- Okumura M, Shintani Y, Funaki S, et al. Right-side approach. Asvide 2018;5:400. Available online: http://www.asvide.com/article/view/24318
- Okumura M, Shintani Y, Funaki S, et al. Left-side procedure. Asvide 2018;5:401. Available online: http://www.asvide.com/article/view/24319
- Caronia FP, Fiorelli A, Santini M, et al. Uniportal bilateral video-assisted thoracoscopic extended thymectomy for myasthenia gravis: A case report. J Thorac Cardiovasc Surg 2015;150:e1-3. [Crossref] [PubMed]
Cite this article as: Okumura M, Shintani Y, Funaki S, Kanzaki R, Ose N, Minami M. VATS thymectomy—bilateral approach for extended resection. Mediastinum 2018;2:37.